Articles
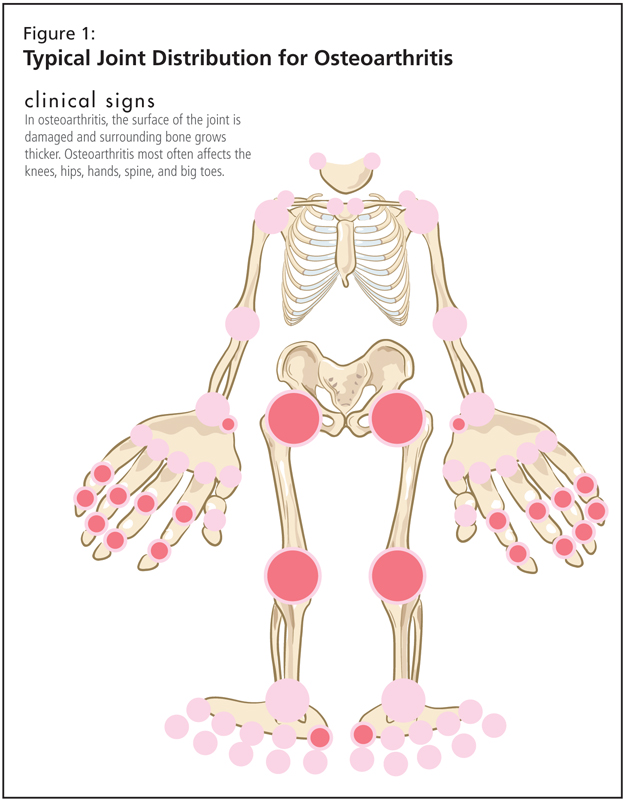
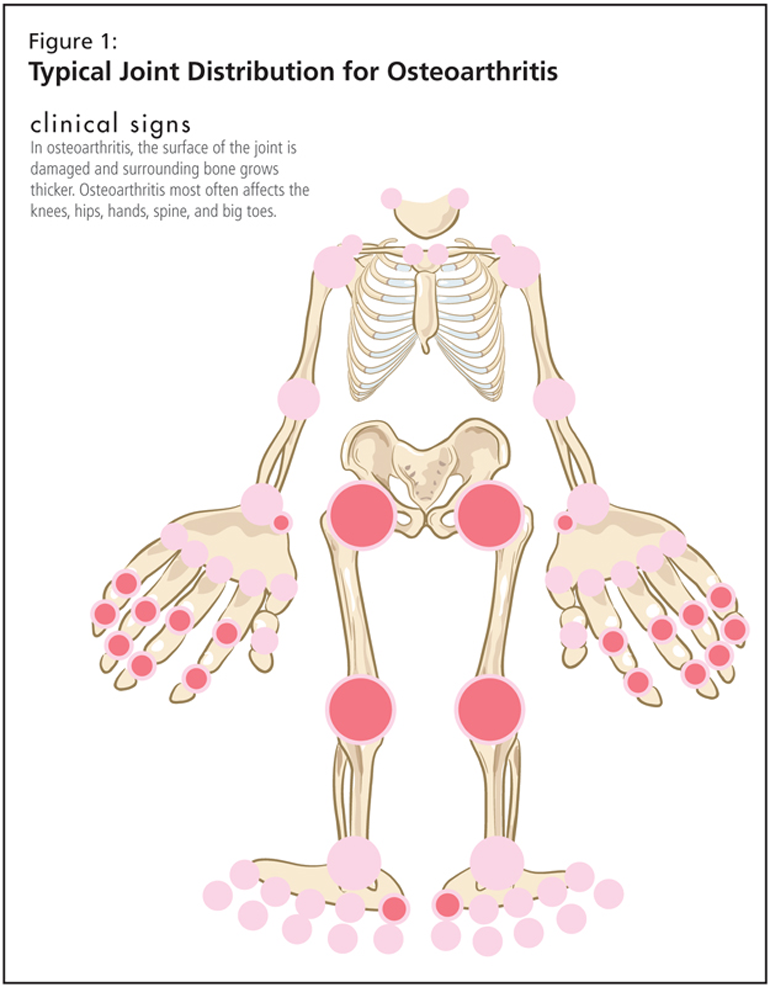
Movement as Medicine in Osteoarthritis

Back Education: Does it Work for Patients?

Quick Facts about Nocturia
Quick Facts about Nocturia
Disclaimer:
This article was published as part of THE LATEST IN THE DIAGNOSIS AND MANAGEMENT OF NOCTURIA eCME resource.
The development of THE LATEST IN THE DIAGNOSIS AND MANAGEMENT OF NOCTURIA eCME resource was supported by an educational grant from Ferring Inc.
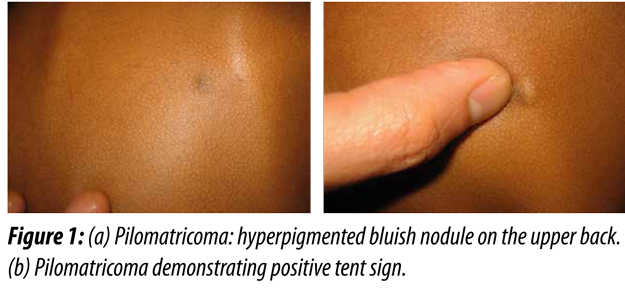
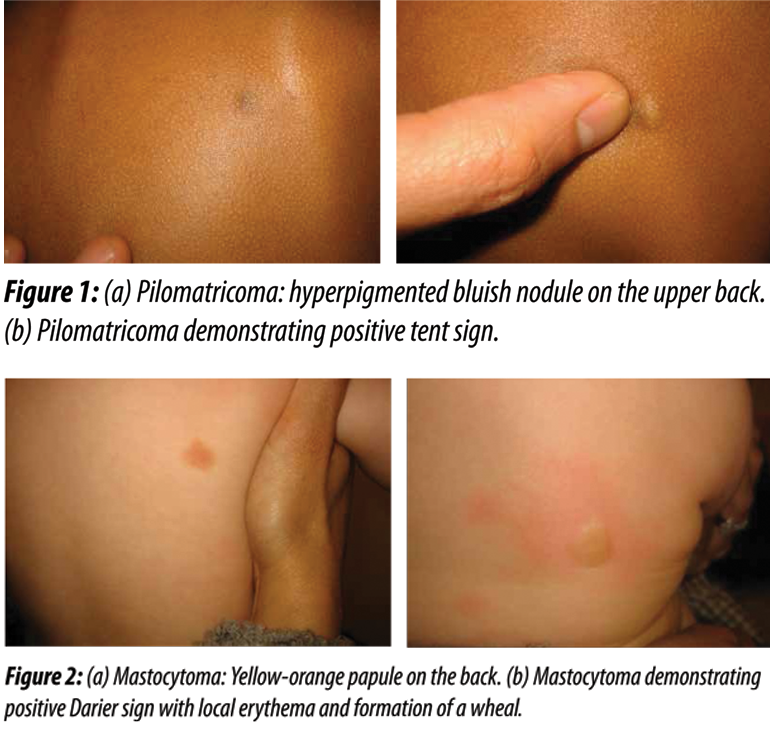
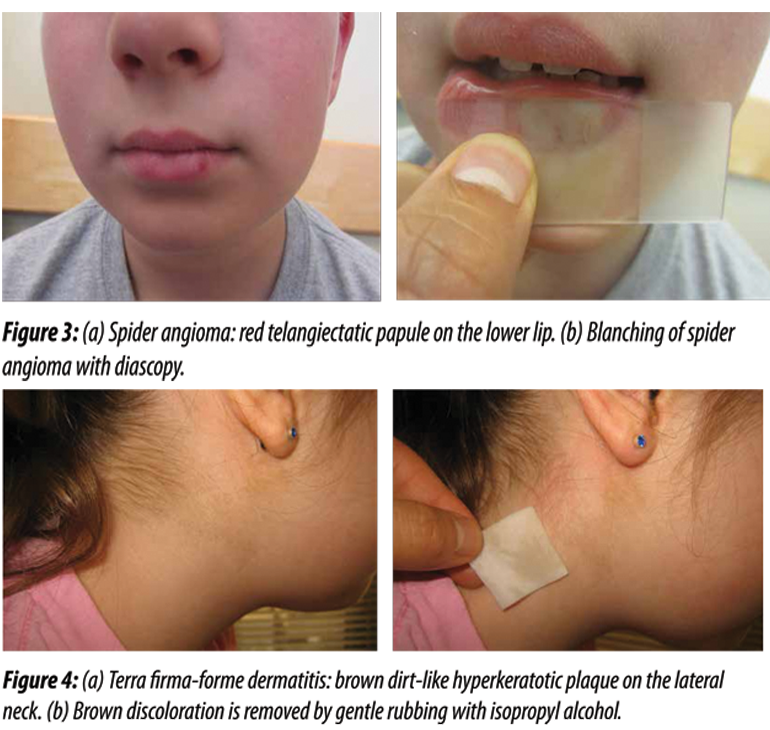
Five Dermatologic Diagnoses at Your Fingertips

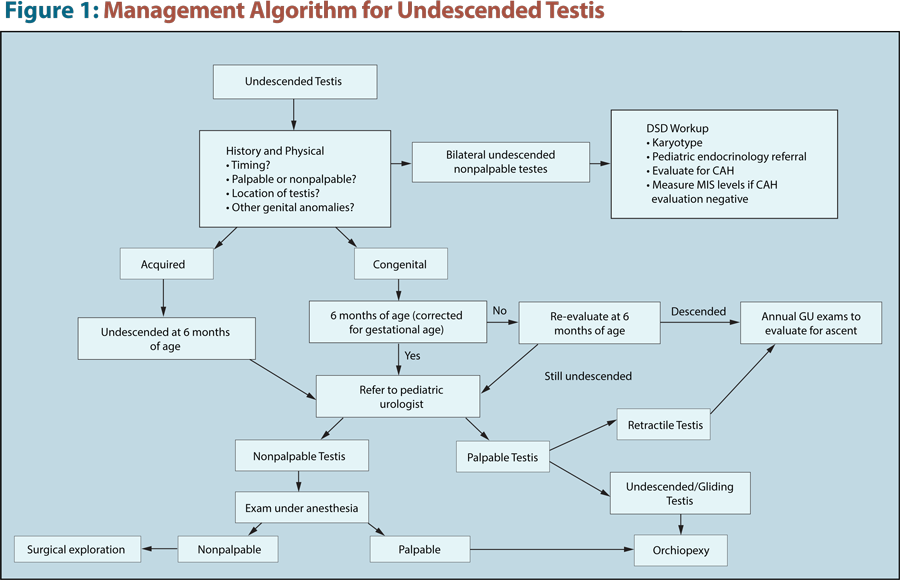
Clinical Management of Disorders of Sex Development

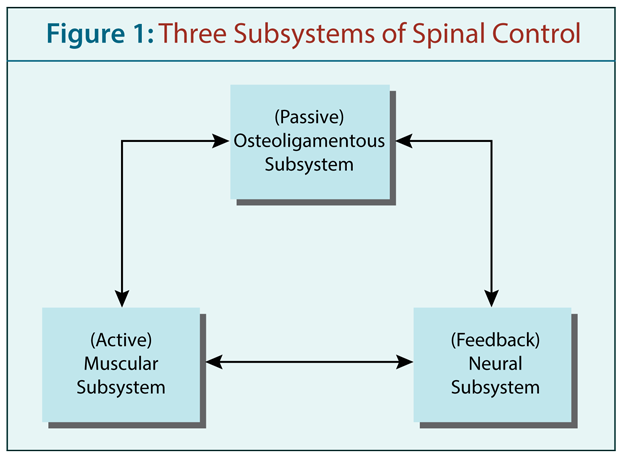
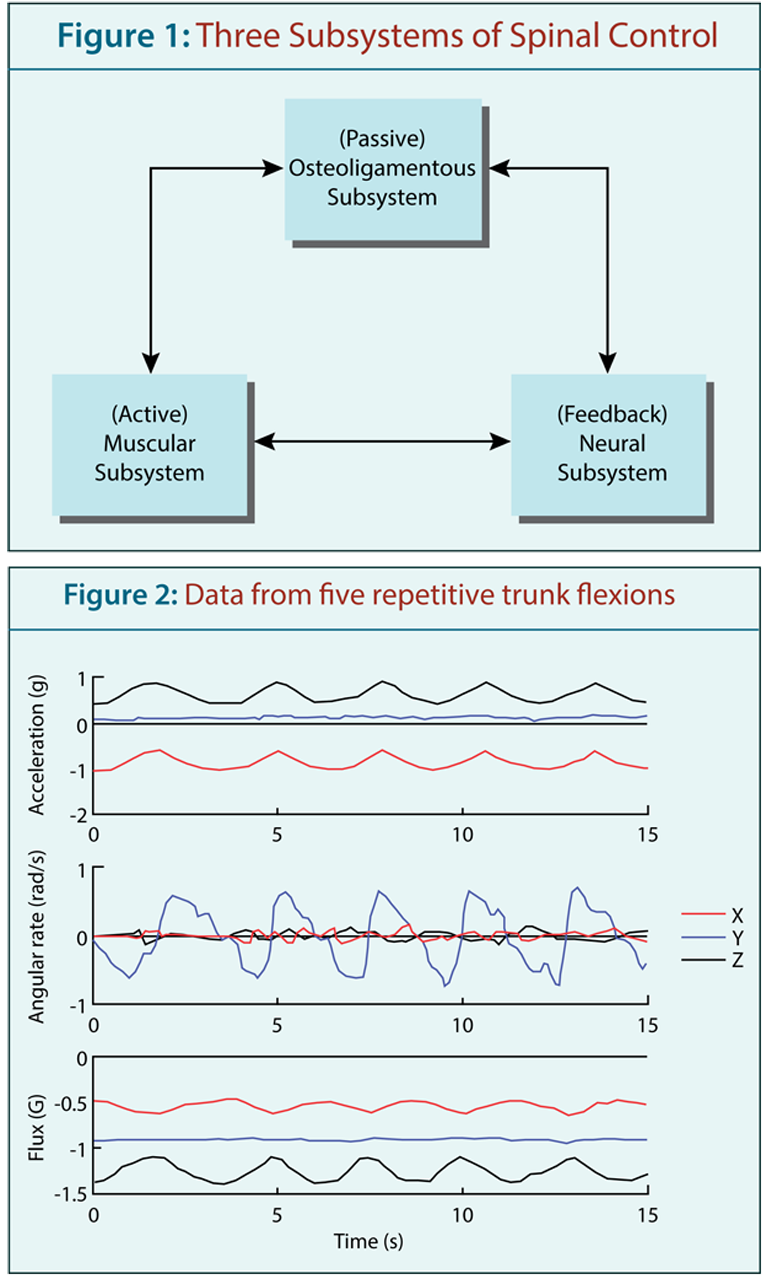
A Spinal Control Approach to Back Pain for the Primary Care Provider

Dementia: Hearing Loss May Contribute to Symptoms

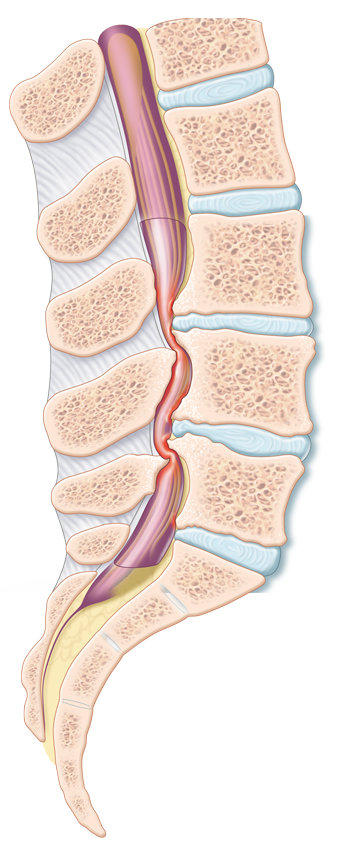
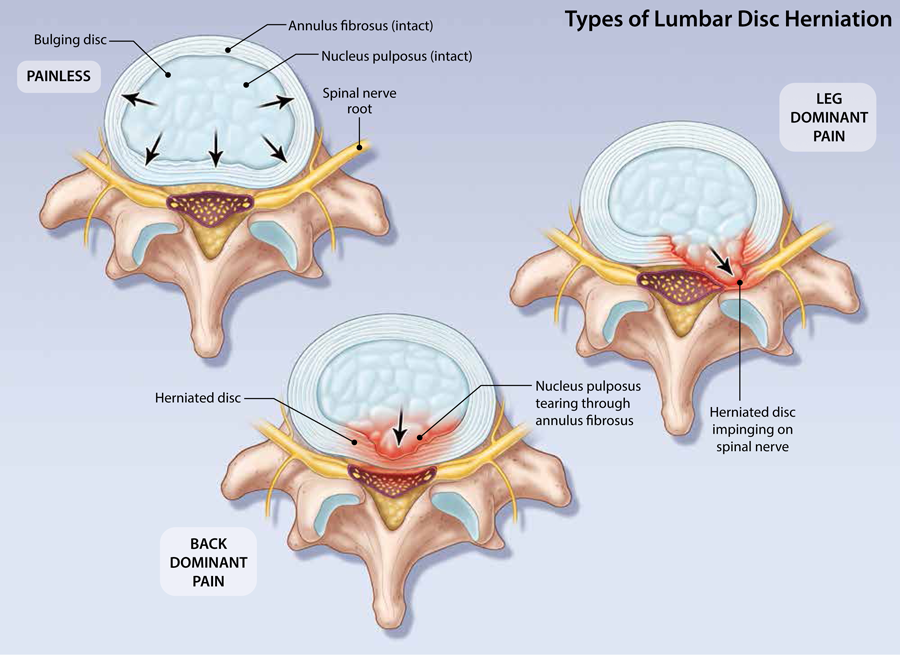
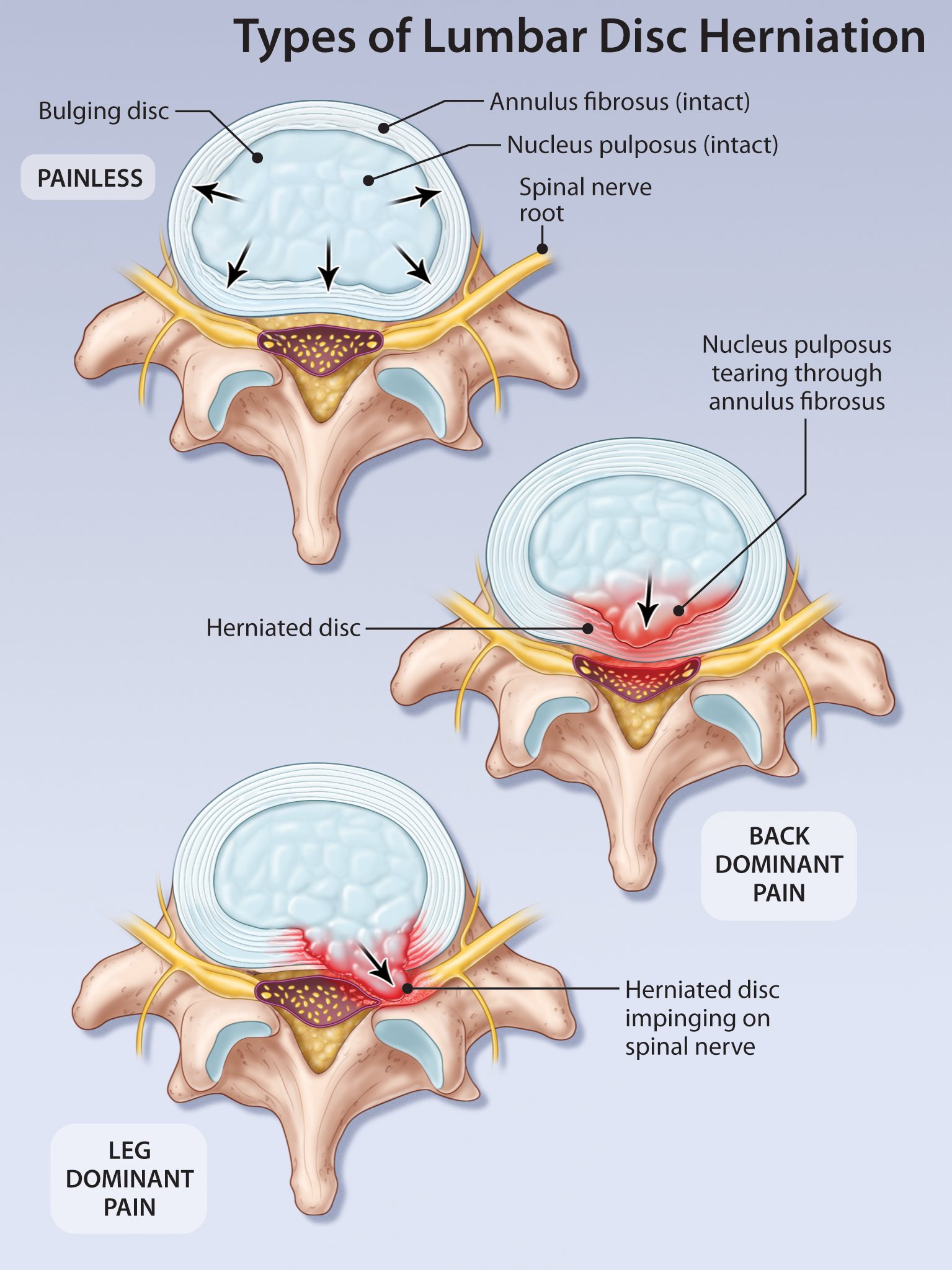
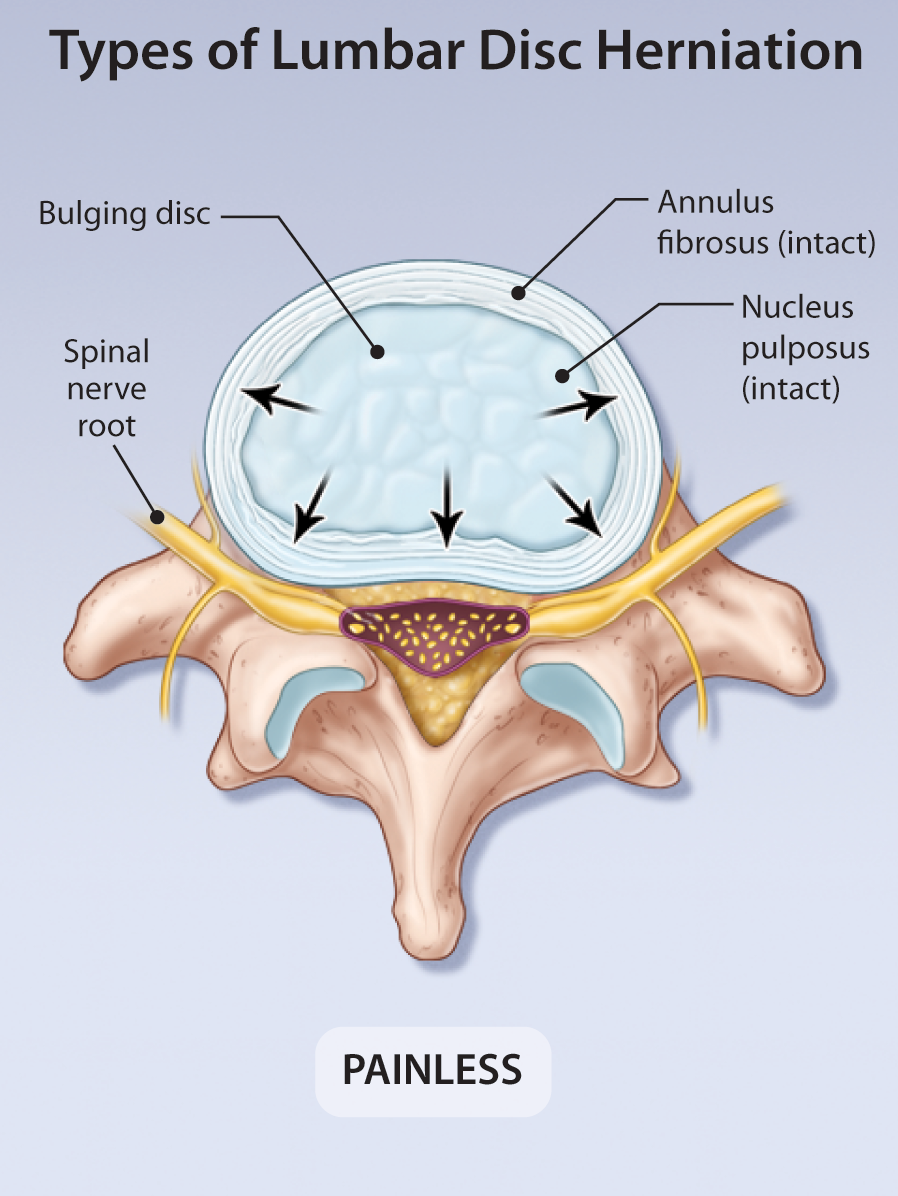
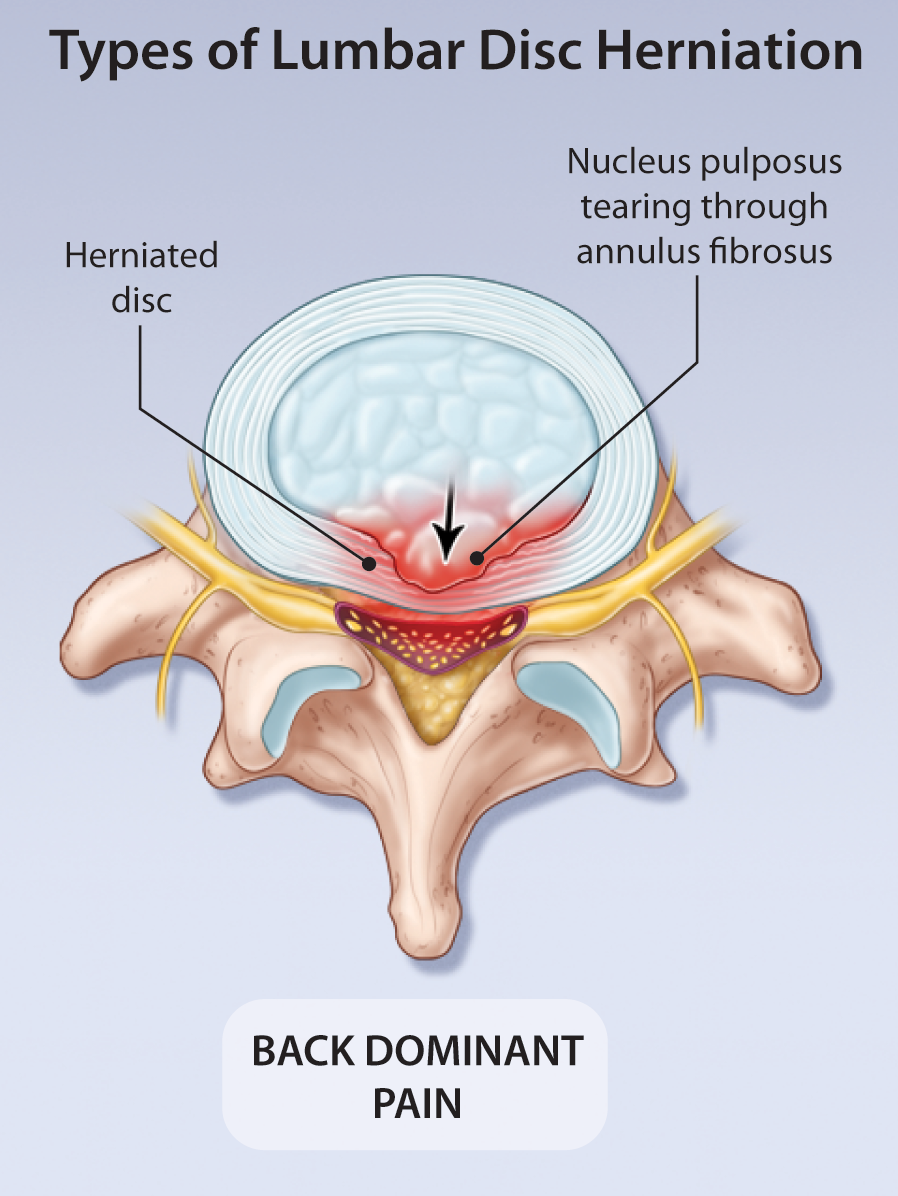
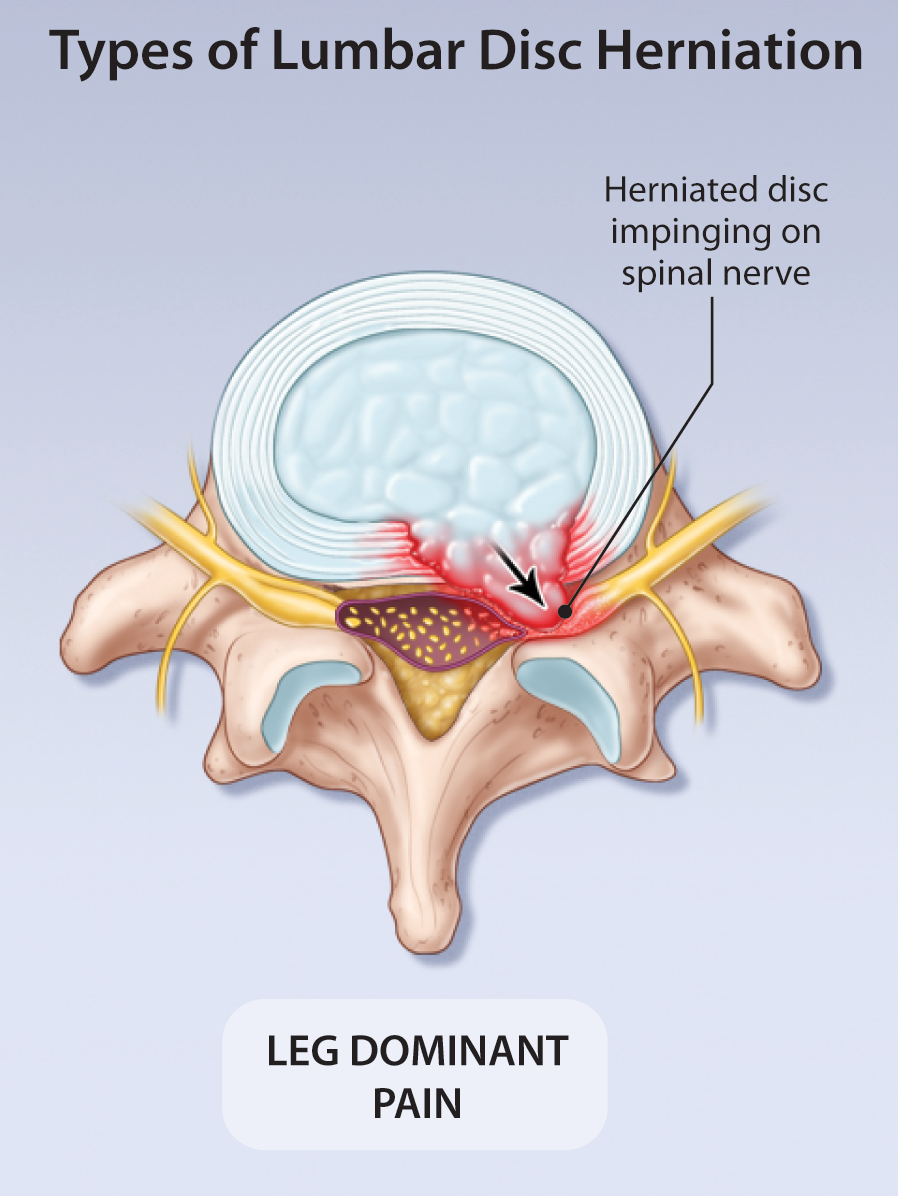
Current Management of Symptomatic Lumbar Disc Herniation

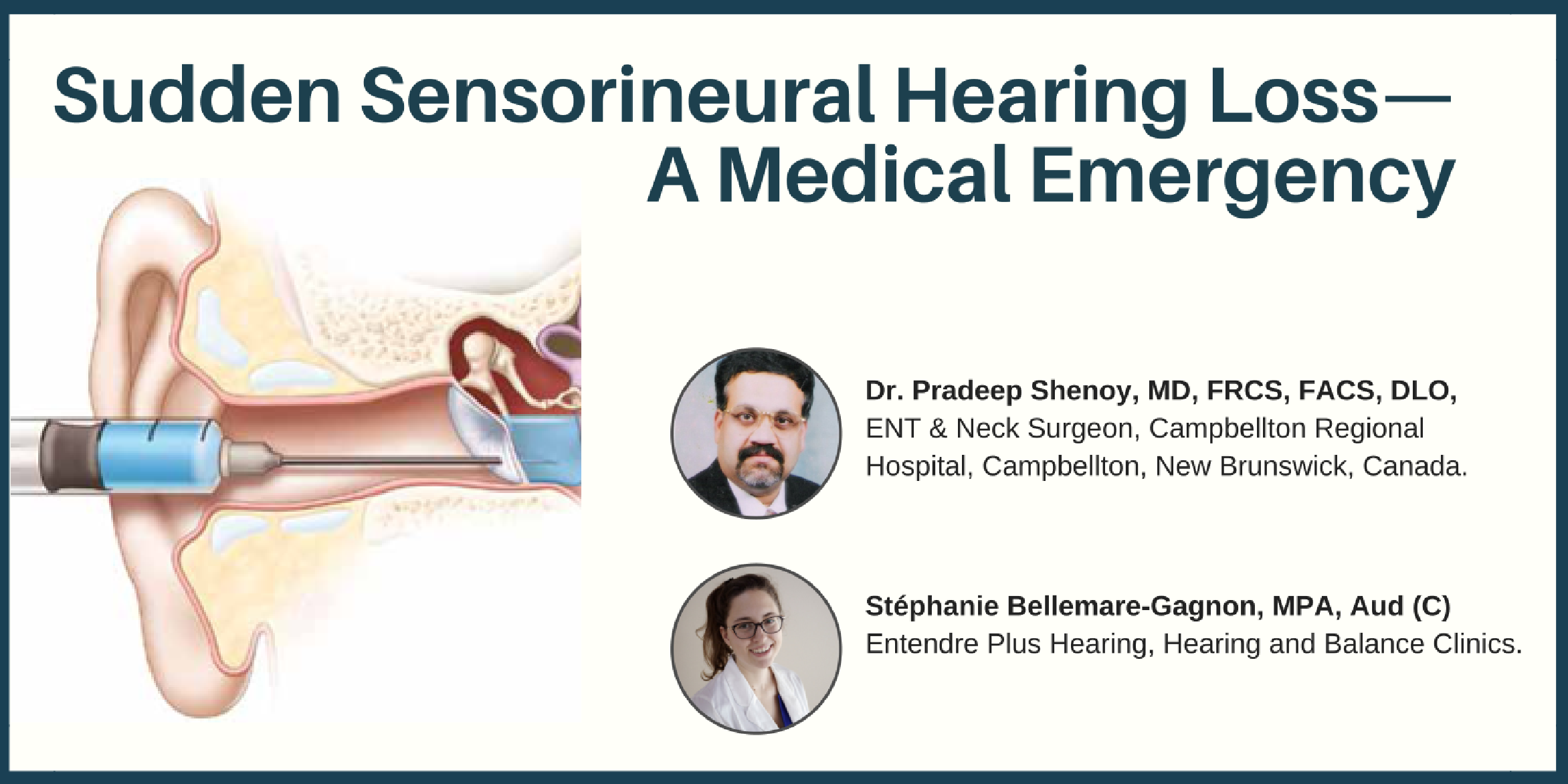
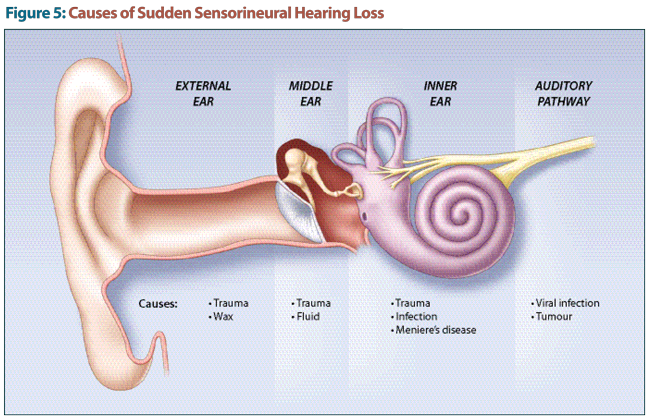
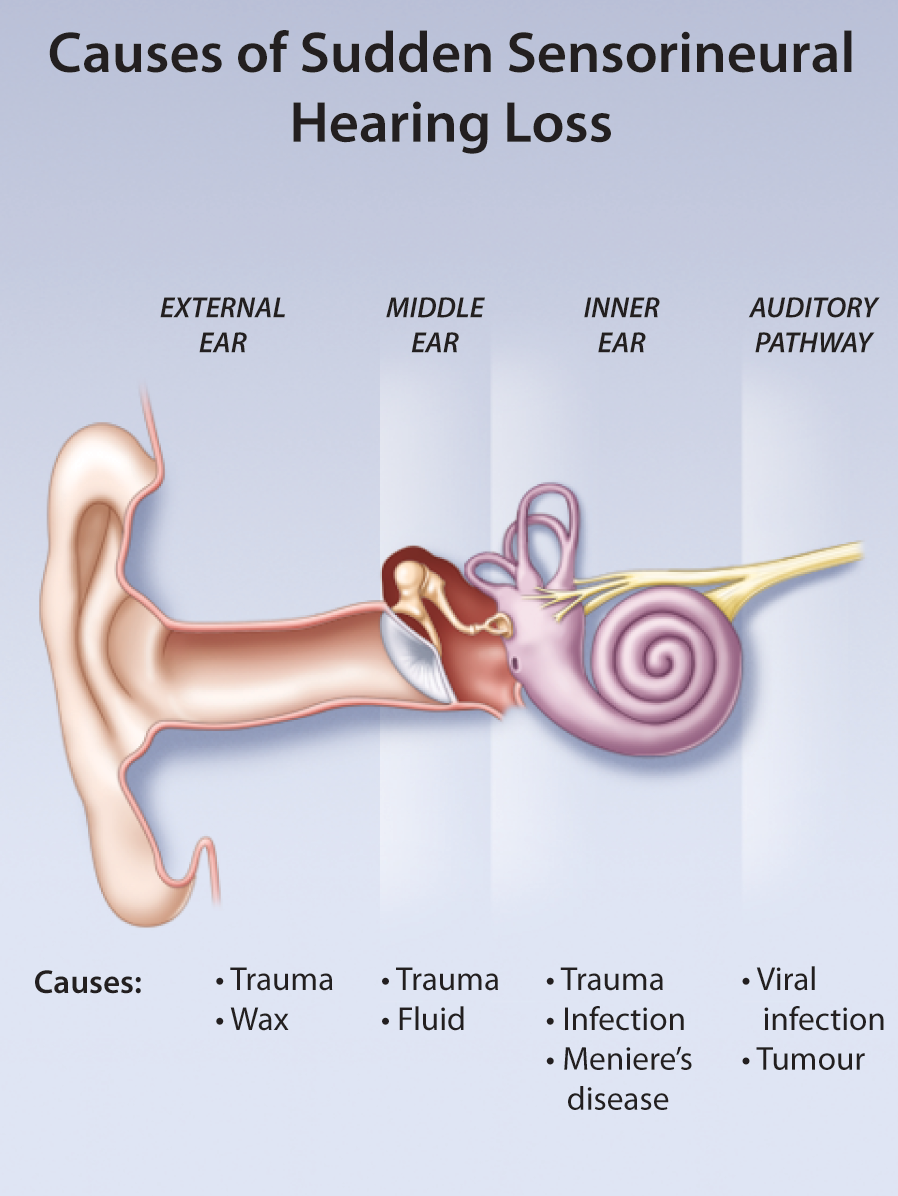
Sudden Sensorineural Hearing Loss—A Medical Emergency