Editor's Note, Volume 6 Issue 1
Editor's Note, Volume 6 Issue 1
D’Arcy Little, MD, CCFP, FRCPC
Medical Director, JCCC and HealthPlexus.NET

- Read more about Editor's Note, Volume 6 Issue 1
- Log in or register to post comments
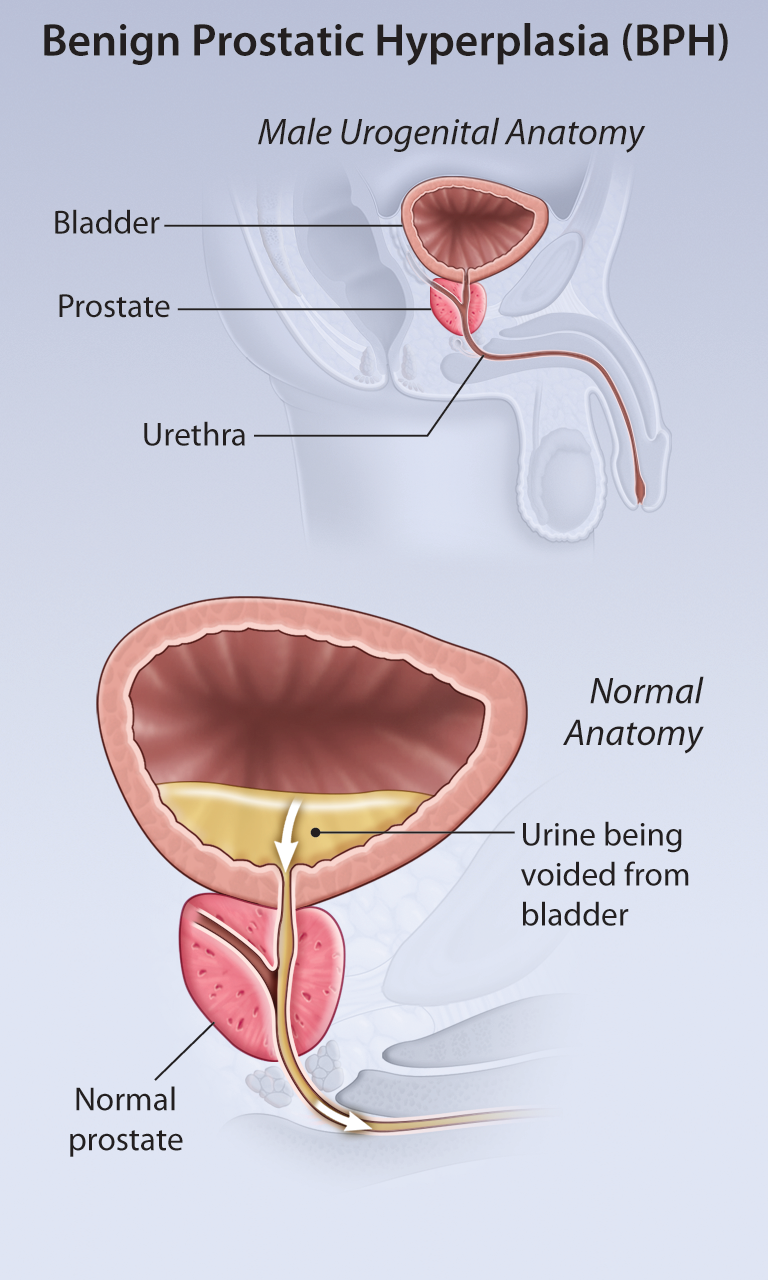
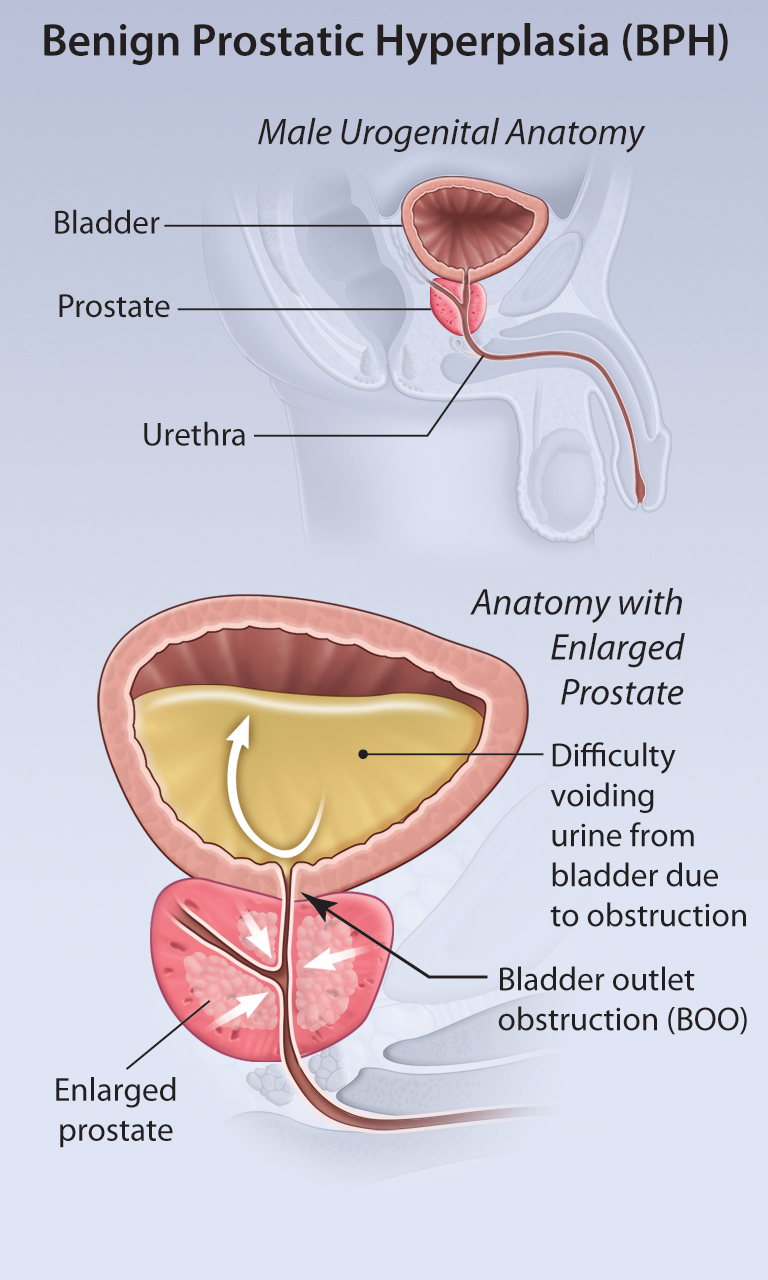
Benign Prostatic Hyperplasia—Medical and Surgical Treatment Options
Benign Prostatic Hyperplasia—Medical and Surgical Treatment Options
Post-test: Benign Prostatic Hyperplasia—Medical and Surgical Treatment Options
| Questions | 3 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Pass rate | 75 % |
| Backwards navigation | Allowed |
You are not allowed to take this Quiz.
Pre-test: Benign Prostatic Hyperplasia—Medical and Surgical Treatment Options
| Questions | 3 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Pass rate | 75 % |
| Backwards navigation | Allowed |
You are not allowed to take this Quiz.
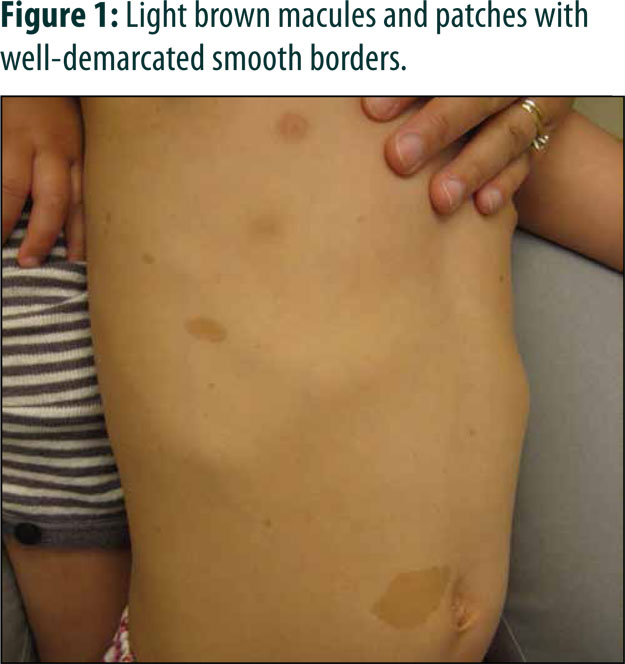
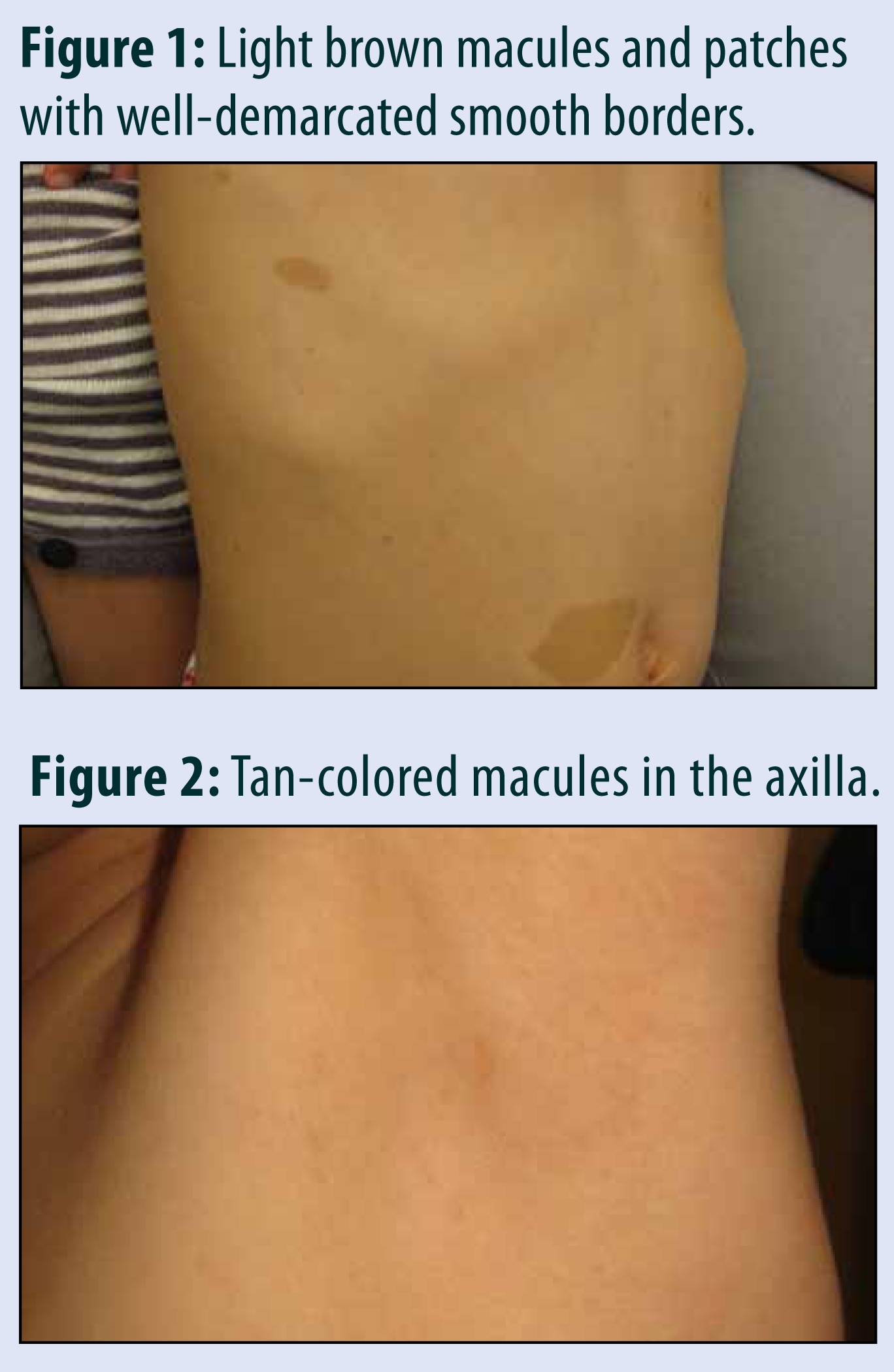
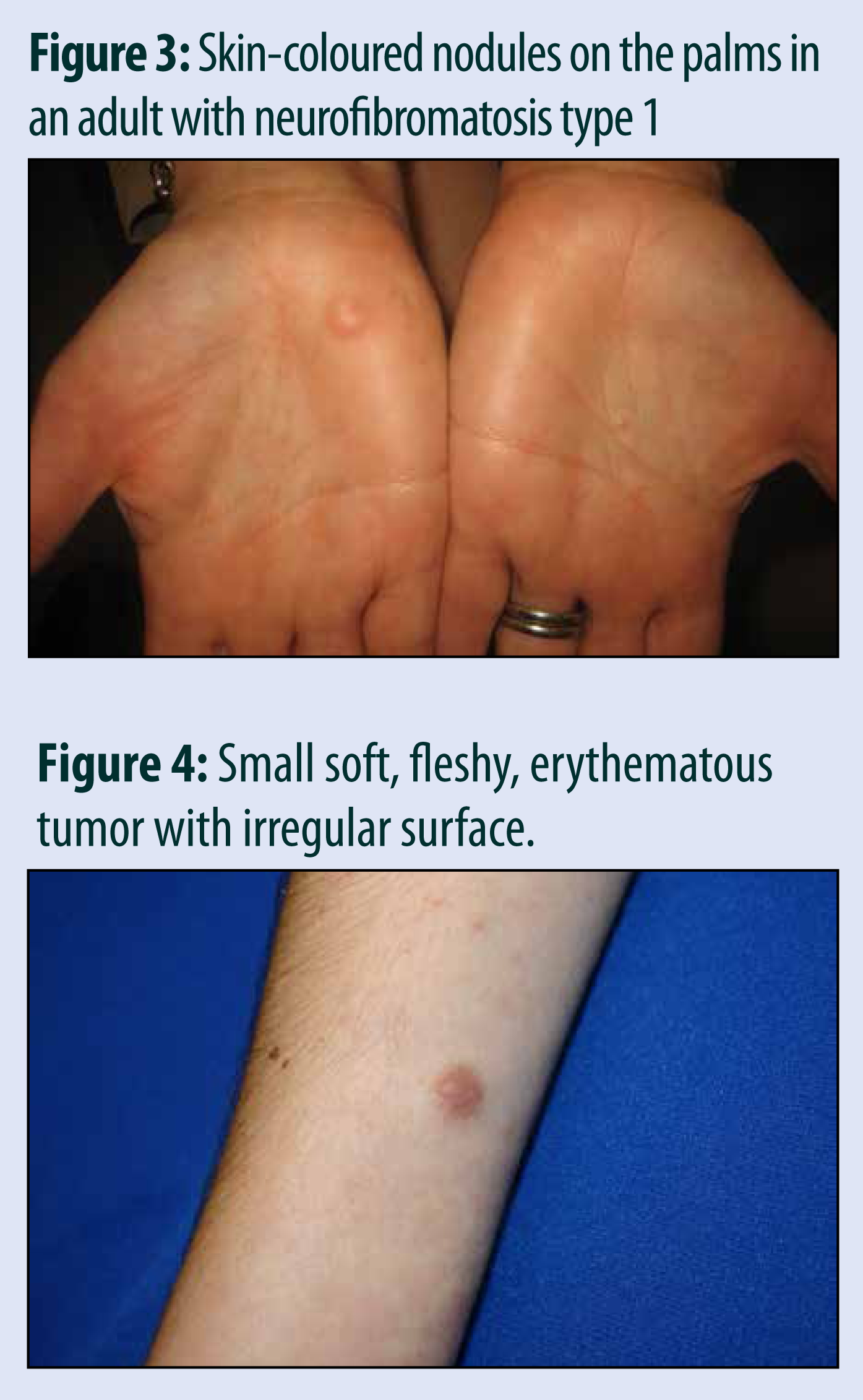
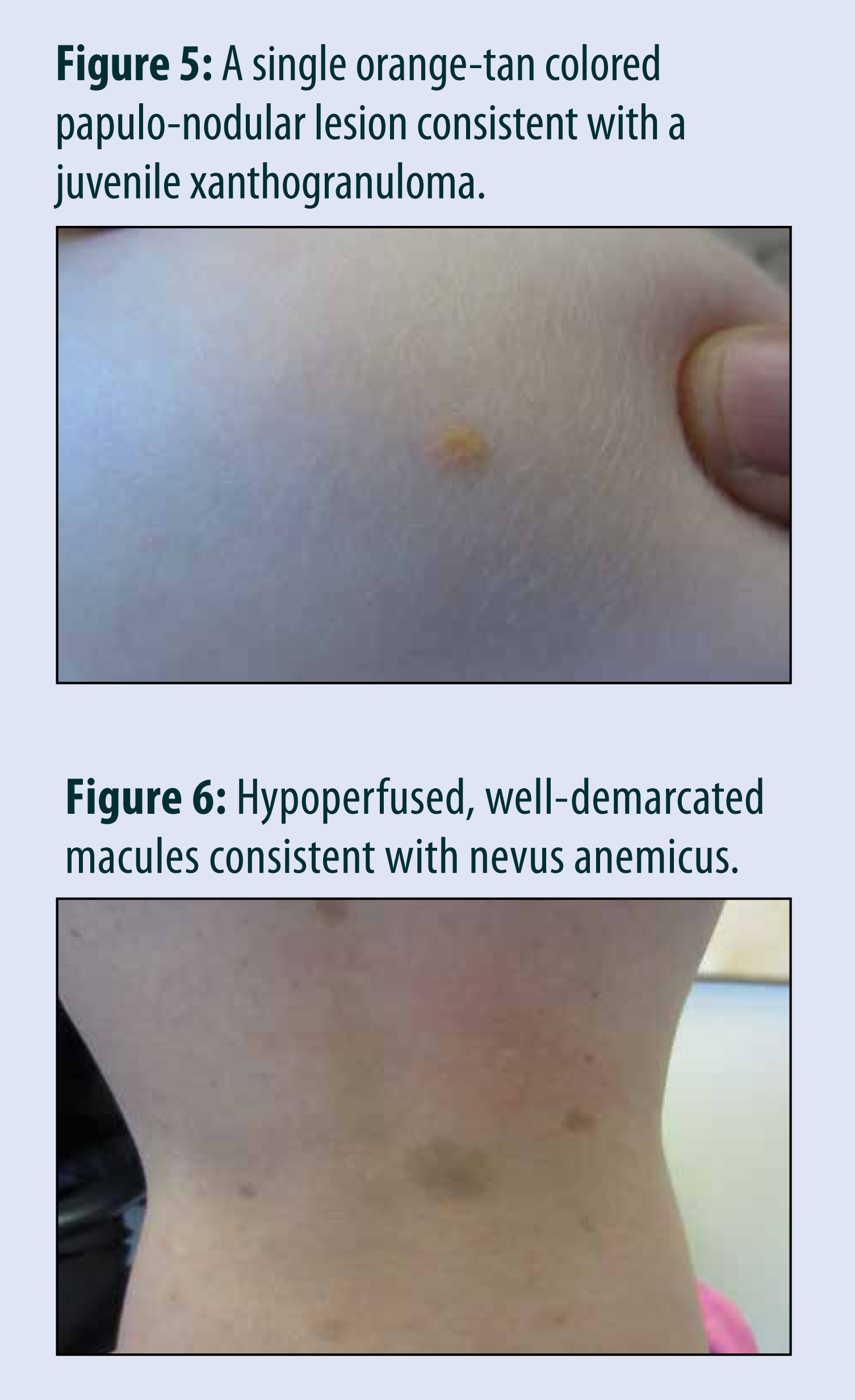
Cutaneous Features of Neurofibromatosis
Cutaneous Features of Neurofibromatosis
Post-test: CORE BACK TOOL 2016: New and Improved!
| Questions | 5 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Pass rate | 75 % |
| Backwards navigation | Allowed |
You are not allowed to take this Quiz.
Pre-test: CORE BACK TOOL 2016: New and Improved!
| Questions | 3 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Pass rate | 75 % |
| Backwards navigation | Allowed |
You are not allowed to take this Quiz.
Post-test: Straight Leg Raise Test
Members of the College of Family Physicians of Canada may claim MAINPRO-M2 Credits for this unaccredited educational program.
| Questions | 4 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Backwards navigation | Forbidden |
You are not allowed to take this Quiz.
Pre-test: Straight Leg Raise Test
Passive Straight Leg Raise Test: Definition, Interpretation, Limitations and Utilization
| Questions | 4 |
|---|---|
| Attempts allowed | Unlimited |
| Available | Always |
| Backwards navigation | Forbidden |
You are not allowed to take this Quiz.