Madhuri Reddy, MD, Dermatology Day Care (Wound Healing Clinic), Sunnybrook and Women's College Health Care Centre, Toronto, ON, Associate Editor, Geriatrics & Aging.
R. Gary Sibbald, BSc, MD, FRCPC (Med), FRCPC (Derm), MACP, DABD, Associate Professor and Director of Continuing Education, Department of Medicine, University of Toronto, Toronto, ON.
Introduction
Pressure ulcers are areas of localized damage to the skin and underlying tissue caused by pressure, shear, friction, excess moisture, incontinence or abrasion. They usually occur over bony prominences such as the sacrum, heels, hips and elbows (Figure 1).
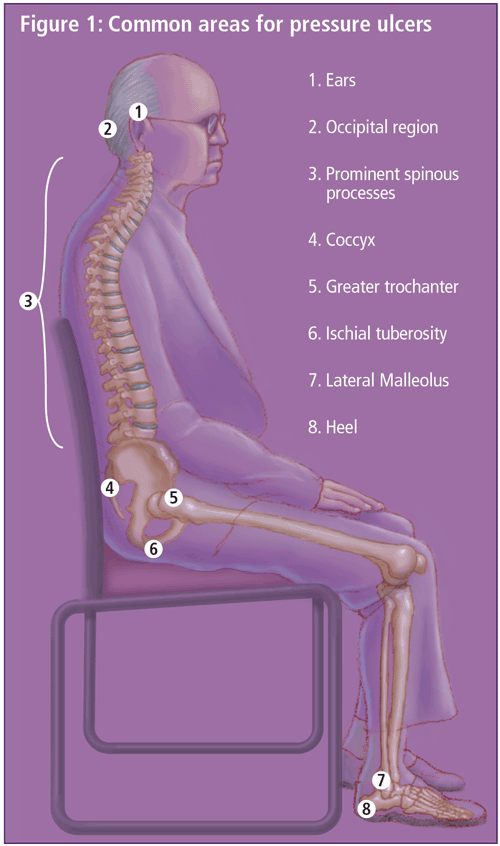
Pressure ulcers are associated with a significant burden of illness in the elderly and a significant financial burden to the health care system. In a recent study of a geriatric unit in Glasgow, the prevalence of pressure ulcers was 41%.1 The incidence in acute care2 has been estimated at 10%, and up to 60% of patients develop ulcers while in acute care hospitals.3 In one study, the prevalence of stage I-IV pressure ulcers in 1,960 acute care facilities in Canada from 1995-1998 was 11.2%.4 The incidence rate for home care is 15.4%.5 Approximately 45% of all pressure ulcers are probably preventable.
Annually, 1.7 million patients in the U.