
Project-Based Quality Improvement Made Successful and Publishable
Speaker: Roger Wong, BMSc, MD, FRCPC, FACP, Department of Medicine, University of British Columbia, Vancouver, BC.
Dr. Roger Wong offered a practical discussion and workshop on project-based quality improvement for geriatrics trainees. Quality improvement is an area of professional aptitude associated with the geriatrician’s role as a manager, one of the seven roles defined by CanMEDS. The CanMEDS framework was created by the Royal College of Physicians and Surgeons of Canada as a resource for medical education, physician competencies, and quality care, which are all predicated on meeting the health needs of society.
Quality improvement (QI) is a core competency for a geriatrician, Dr. Wong explained, and central to the objective of becoming a better physician and offering better care to older adults. Dr. Wong aimed to provide an overview of QI.
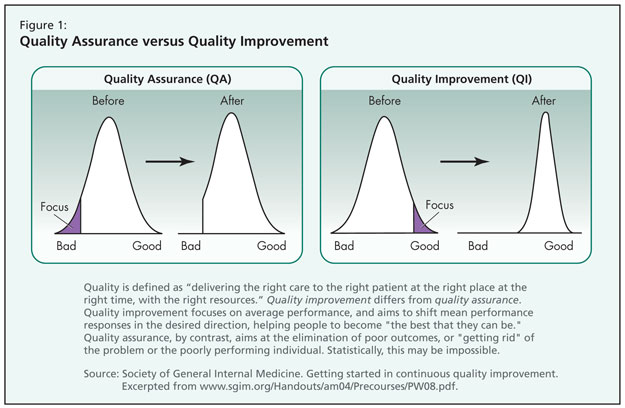
He defined quality as “delivering the right care to the right patient at the right place at the right time, with the right resources.” Quality improvement differs from quality assurance in its focus on shifting an entire outcome curve toward an explicitly defined aim, an aim that is achieved through an intentionally planned and executed model of improvement (Figure 1). Rather than aiming at the elimination of poor outcomes, QI implementation focuses on average performance and aims at building on functional success, identifying what works in an organization and empowering members to perform their best.
As a framework for facilitating improvement, Dr. Wong presented an approach to improving organizational performance through the PDSA model, or “plan, do, study, act.” Planning pertains to setting aims; doing defines actionable measures; studying involves targeting areas of change; and acting denotes implementing and testing changes.
Dr. Wong then spoke to the attributes of an effective QI team. Such a team recruits leadership with the authority and/or influence to institute change; involves team members with clinical expertise, who understand the problem at hand and QI principles; and appoints day-to-day leaders capable of directing the course of the QI project.
He then offered a tutorial in establishing aims, defined as clear, concise, population-specific objectives; importantly, this phase of QI also involves defining a measurable outcome—one that stretches beyond the status quo while remaining reasonable in the context—to be met within a dedicated timeframe. Good aims endeavor to ensure that participants experience the aims as meaningful and measurable so that they do not drift from adhering to the QI plan. He cautioned that too-broad objectives necessitate refocusing and working on a smaller part of the system first. A meaningful aim in the geriatric context might be setting a particular blood glucose target for patients in a diabetes management program (e.g., “Within the next 12 months, 80% of our diabetic clinic patients will have documented hemoglobin A1c levels of 7.0%.”).
Once a meaningful aim is set, flowcharting focuses on the steps of a process. Precisely documenting a problem helps to identify areas that might be overlooked as potential areas of improvement. The flowchart, he emphasized, must focus on a clinical process and not the entire medical care system; avoid excessive details; include all principle steps in the existing clinical process; and reflect the process as it actually occurs. The objective in flowcharting is to look for areas of error, transitions, conflict, confusion, delay, or hassles in the process. It should include multiple measurements, including outcome (how the system was found to perform), process (whether parts or steps in the system performed as intended) and balancing measurements (whether changes designed to improve one part of the system cause problems elsewhere, e.g., does reducing hospital stays result in higher readmission rates?).
Noting that all improvements require change, Dr. Wong reminded listeners that the PDSA method is a way of testing whether the changes implemented have indeed led to improvements.
The second phase of Dr. Wong’s presentation involved instruction in improvement tools. He reviewed how to establish a project charter, wherein performance improvement goals can be presented in a chart that tracks goals, aims, timelines, leadership, and needed support.
Dr. Wong then discussed sampling (data collection) for PDSA and distinguished between systematic sampling, which collects data at a fixed time or at counted intervals and is useful for high-volume processes, versus block sampling, which selects samples in predetermined size blocks and yields time-dependent data. Such projects involve determining how much data to collect as well as how to present it. He cautioned that data presented in aggregate form can obscure variation in data over time and thus hamper judgment of QI strategies. In assessing data, he emphasized distinguishing between common cause variation (internal to the system; repeatable; influenced by chance) versus special cause variation (unusual and traceable to circumstance). The appropriate course of action will be dictated by the variation type.
The final portion of the workshop involved guidance in identifying valuable project areas in medicine, particularly those with an impact on geriatric care. Valuable QI projects might involve interventions to reduce error, manage time, eliminate waste, or improve clinician/patient interactions. Team projects in geriatrics could involve medication transitions (e.g., moxifloxacin step-down from IV to oral therapy) or facilitating continuity of care (e.g., studying effects of informational faxes to family doctors post-hospitalization). He encouraged trainees to think about areas of improvement in their local contexts, and before concluding engaged workshop participants in an exercise, devising a QI project and producing an aim statement.
In planning team projects he advised careful attention to project magnitude. Project leaders should ensure the magnitude is manageable, that participants are prepared to manage negative results, that adequate time is allotted for QI activities, that communicative skills are engaged, that stakeholders are integrated into the project, and that there is longitudinal follow-up to ensure team members are on track. Dr. Wong reminded the audience that commonly accepted guidelines for publishing QI projects exist (e.g., Standards for Quality Improvement Reporting Excellence [SQUIRE], online at www.squire-statement.org).


