Movement Disorders
Music and Movement....Disorders
When one thinks of music and movement, the natural association is dance. In all parts of the world and in all cultures, there is some musical expression through dance, ranging from what may appear to be relatively simple rhythmic movements to compelling drum beats to complex ballets with narratives and dozens if not more dancers doing intricate steps to full blown orchestras. Anyone that has raised children recalls how even very young children, will move and shake to rhythmic music and the massive industry in all western countries of dance lessons starting with child students attests to its natural attraction and ability to fulfill what appears to be an intrinsic human desire.
I recall as a child being taken to ballet, modern dance, musicals with dance and even the renowned Rockets at the Radio City Music Hall by my mother who herself had been a serious amateur dancer in her youth and then a lifelong ball-room and late-life folk dancer with her seniors' centre on West End Avenue in Brooklyn. There was even a period of my pre-teen years when my mother attempted to teach me ballet steps at home which very soon was transposed into my desire to learn to dance to Rock and Roll, using my sister four years my junior as my every accommodating dance partner. Even many years after, in our mature and pre-senior years, at family celebrations we often could still do a dance number to something of the order of Rock Around the Clock or the theme song for Saturday Night Fever. She has continued to engage with multi- cultural folk dancing whereas I have slowed down considerably in my abilities to participate although I enjoy watching others, dance especially my children and more recently my granddaughters.
The general assumption probably held by most individuals that with physical and especially neurological disability, the ability to engage or think about participating in dance would likely naturally diminish. For people living with conditions that impose physical challenges to free and fluid movements, the idea of dancing is more often a dream than a reality. It is likely that it would not even enter the consciousness of most people with neurological disorders, especially those like Parkinson's Disease might be able to participate in, respond to and benefit from music, especially when it is within a framework of dance.
With this in mind the recent article in October 25th issue of The Globe and Mail, by Gayle MacDonald, "Unlocking the secret of Dance" was exhilarating and inspiring. In a partnership with the world-renowned Canada's National Ballet School, with the collaboration and influence of some its most prominent members and in a cooperative effort with among others Toronto's York University and my own Baycrest Geriatric Health Care System, it is hoped that in addition to the great joy satisfaction that all the participants appear to be getting from the program, scientific research studies will demonstrate the mechanism of responsiveness and hopefully clinical improvement.
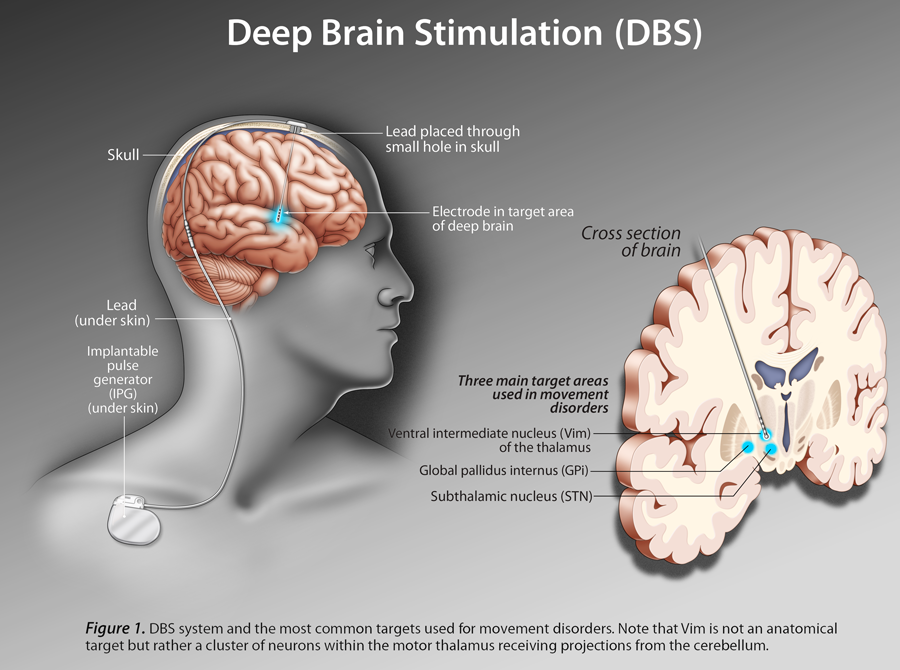
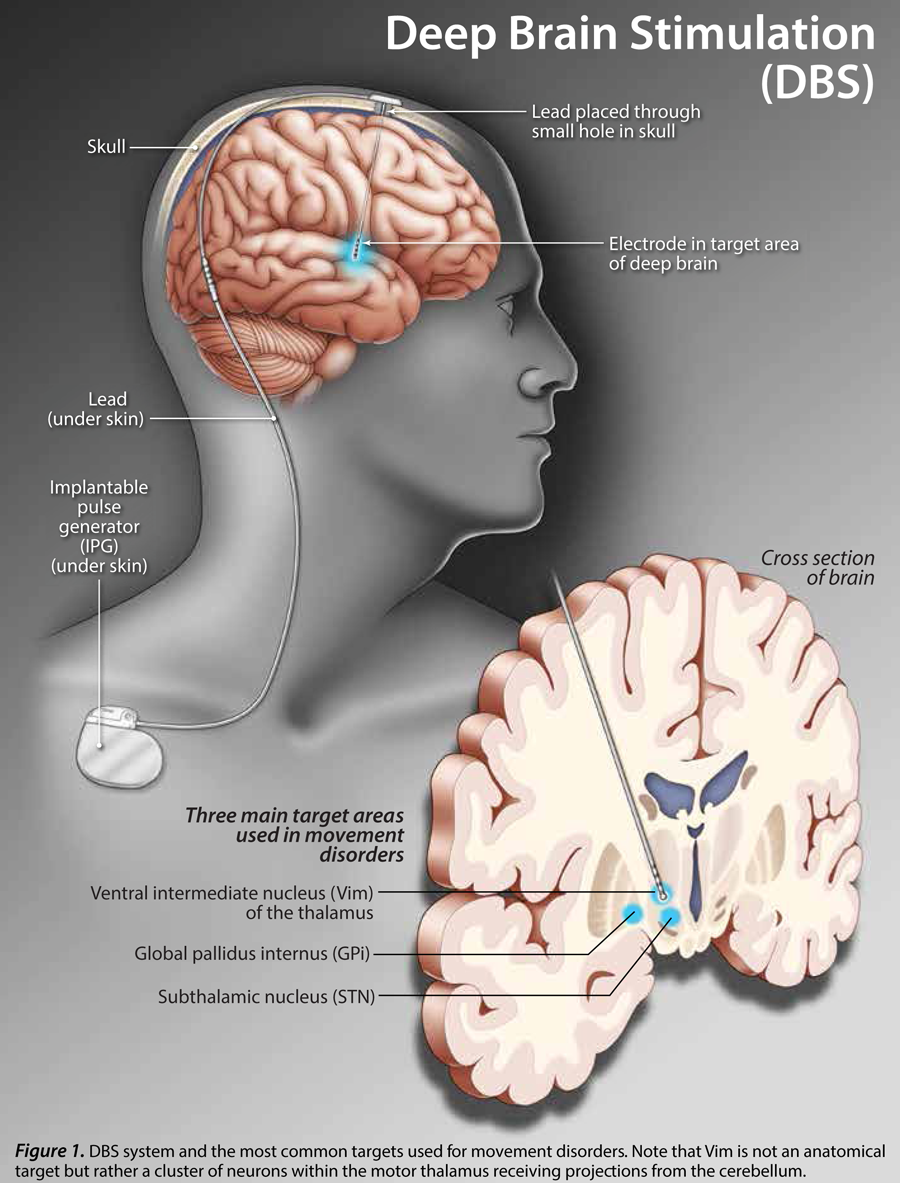
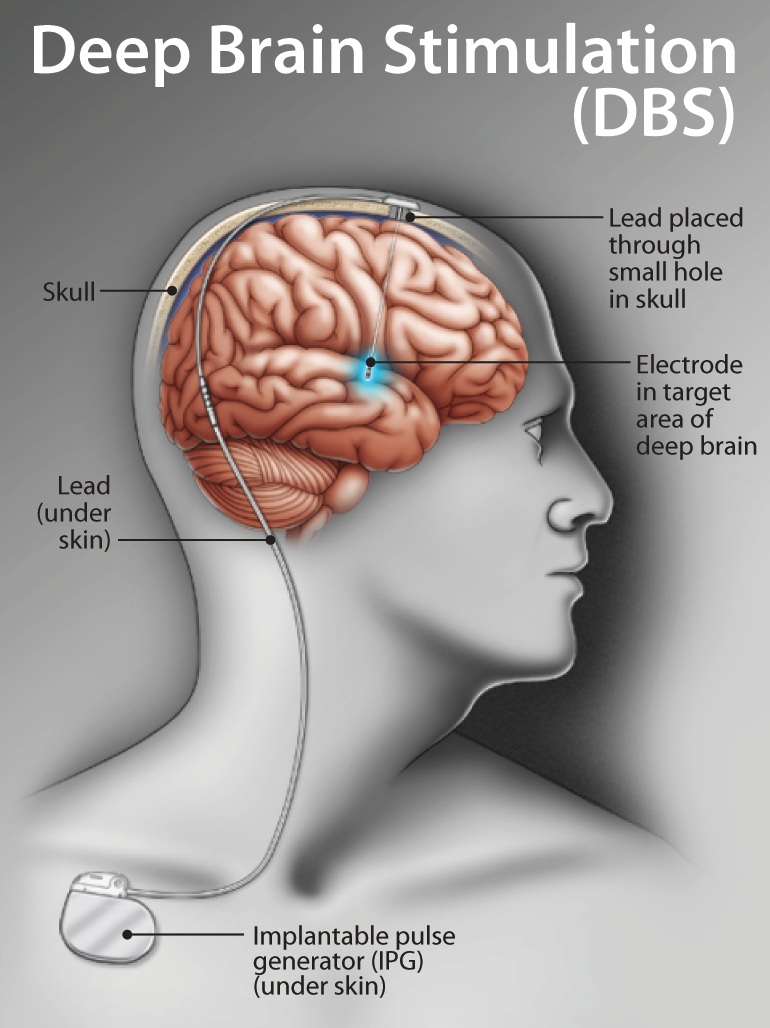
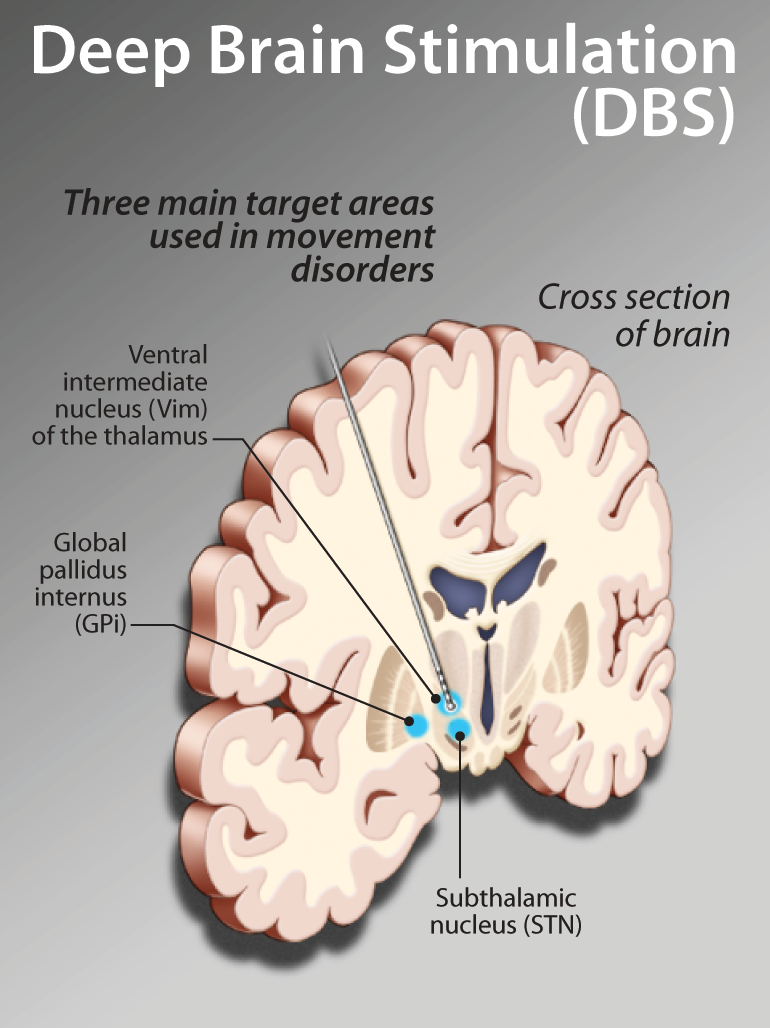
Dance appears to provide a number of benefits to those living with Parkinson's disease which affects seven million people world-wide including approximately 100,000 in Canada and a million people in the United States. It has been established that dance improves characteristics like balance, gait, posture and other physical measurements beyond the social joy and satisfaction from what is in essence a group and social undertaking. Studies are underway to try and determine what the dance does to the brain and the mechanisms by which improvements may occur and whether or not they are sustainable and may be an important adjunct to commonly used medication therapies that are not without their problems.
It has been well known for many years that those living with Parkinsonism can improve their gait by listening to rhythmic marching-type music and some have learned to use ear-phone-directed march music from iPods and other similar devices to provide the compelling rhythmic background to assist in their walking. (Neuroscience and Biobehavioral Reviews: Into the groove; Can rhythm influence Parkinson's disease? Cristina Nombela, Laura E. Hughes, Adrian M. Owen, Jessica A. Grahn, 2013. http://www.ncbi.nlm.nih.gov) In my own practice I have often taken my patients with such movement disorders and while walking with them up the corridor outside my office I hum loudly a well-known John Philip Sousa March, The Stars and Stripes Forever which most people recognize. Quite a lot of the patients and the family are amazed how all of a sudden the person who had been struggling with gait and speed would be walking alongside me to the loudly hummed musical refrain. If the result is good I instruct the person or family member to get some recordings of such marches or others if they are ones that resonate and put them on an iPod type device and place the march when the person wants to go for an enjoyable walk, for the purposes of actual exercise, or as one might in a garden or along a neighbourhood street.
If this Parkinson's ballet dance project proves successful it may result in a wide range of programs that bring dance and music to many individuals living with Parkinson's disease and provide a creative and satisfying and in many ways liberating enterprise for them.
Identification and Management of Impulse Control Disorders Among Individuals with Parkinson’s Disease
Identification and Management of Impulse Control Disorders Among Individuals with Parkinson’s Disease
Members of the College of Family Physicians of Canada may claim one non-certified credit per hour for this non-certified educational program.
Mainpro+® Overview