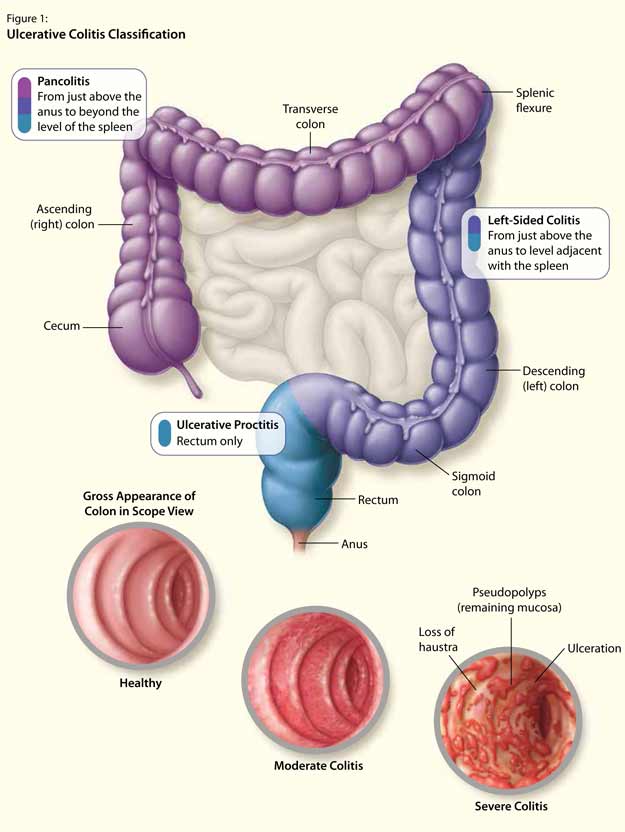
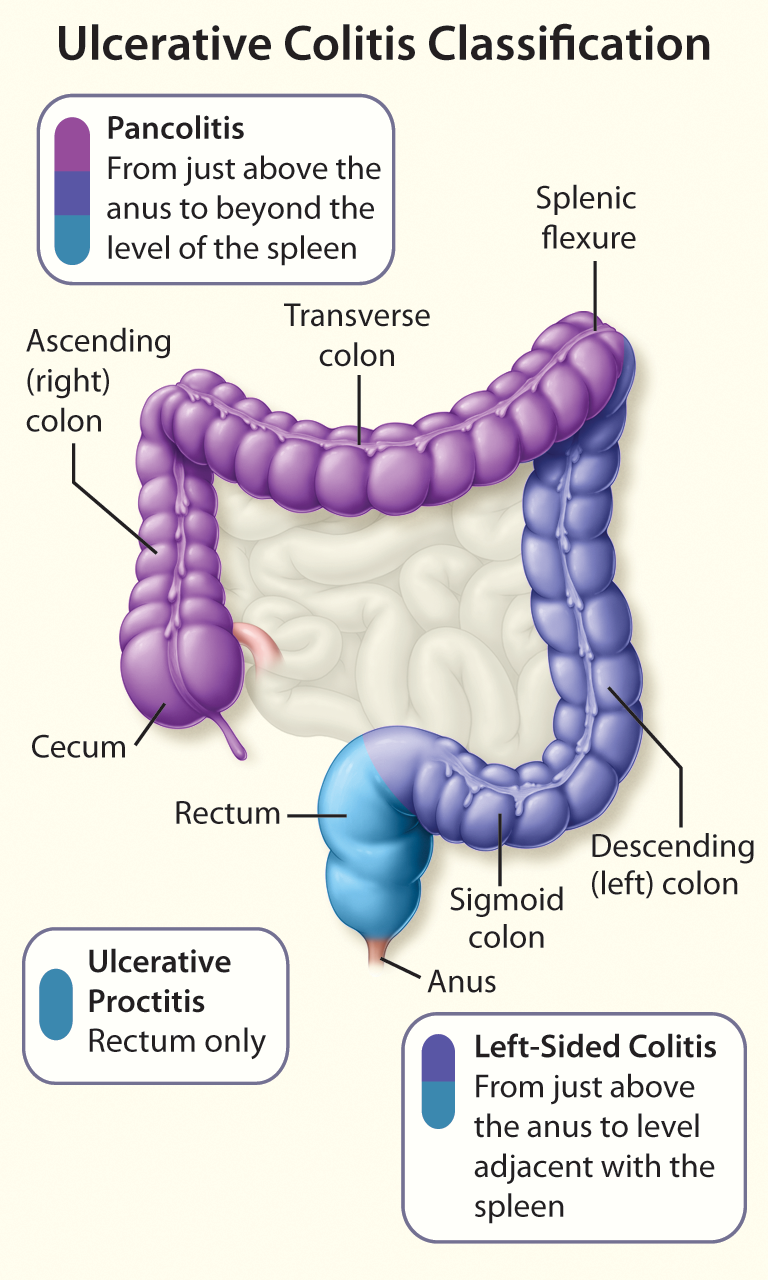
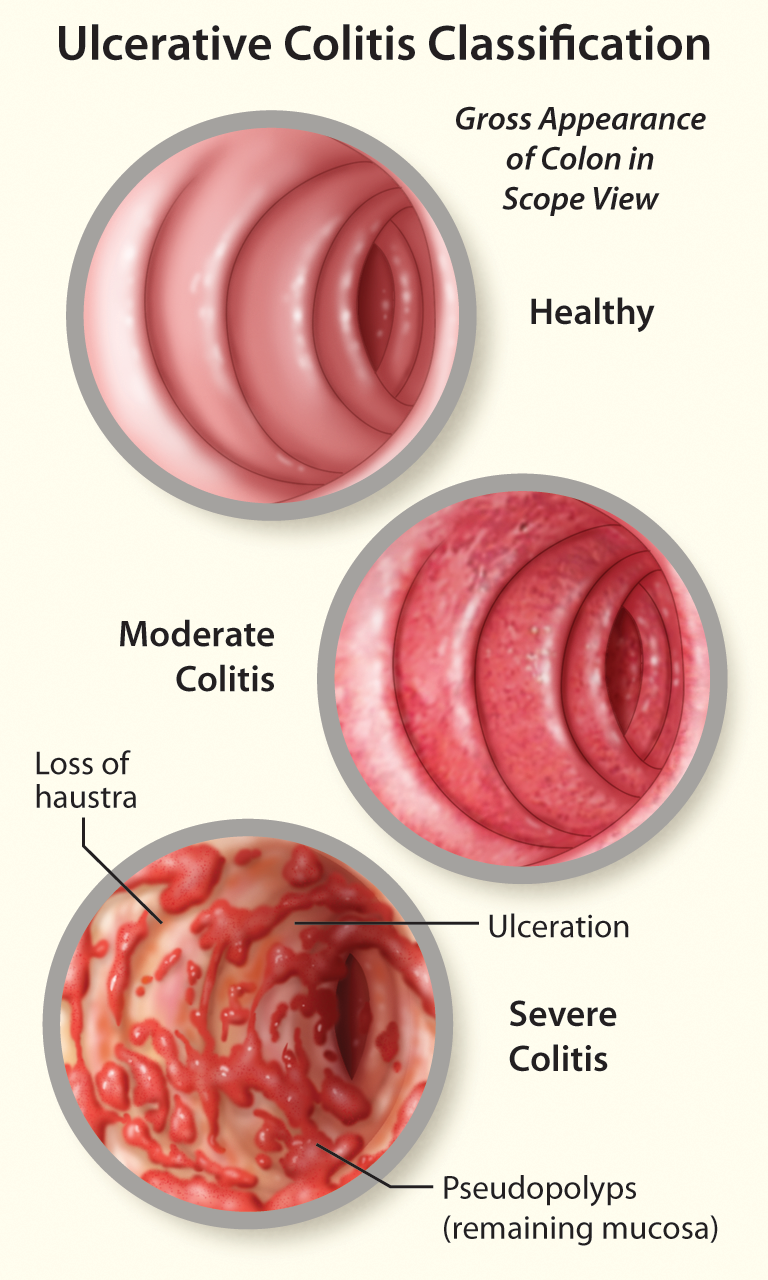
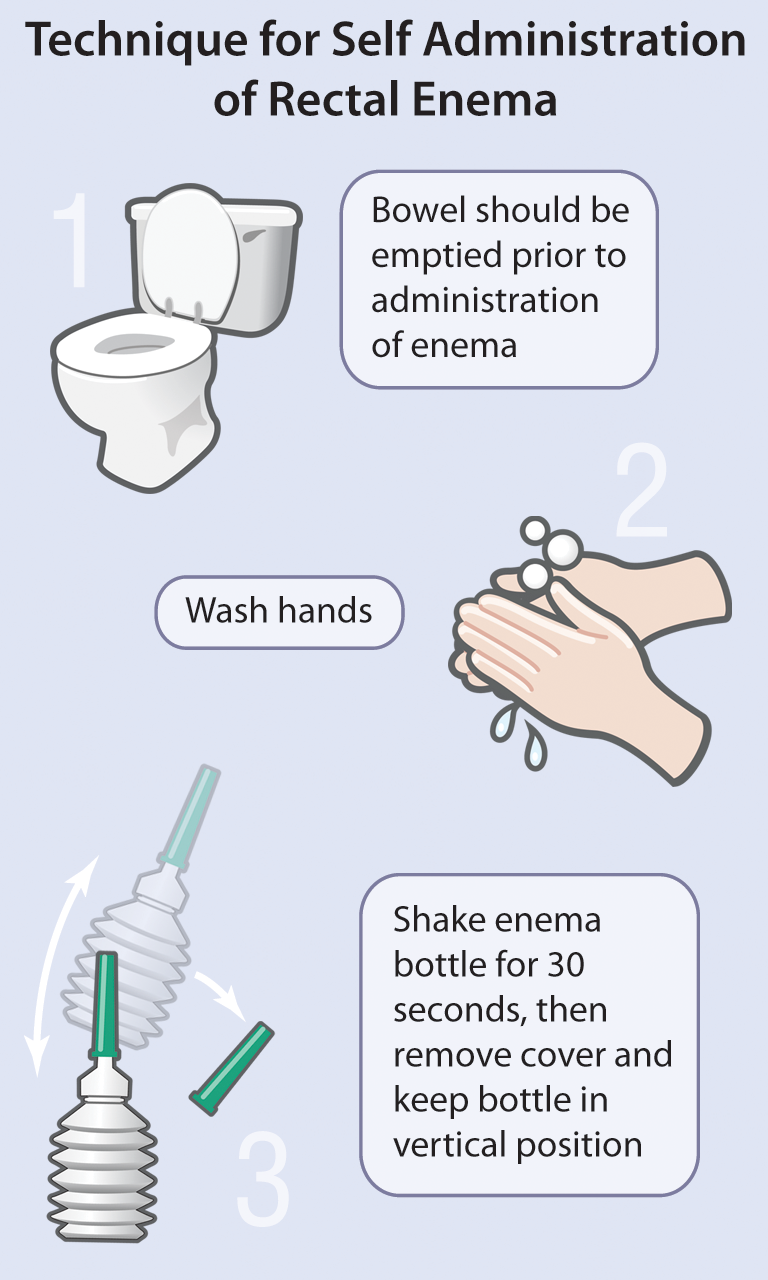
Comprehensive Patient Care in the Treatment of Ulcerative Colitis
Comprehensive Patient Care in the Treatment of Ulcerative Colitis

Marc Bradette, MD, FRCPC, CSPQ, Clinical Professor, Department of Gastroenterology, Pavillon Hôtel-Dieu de Québec, Québec, QC.